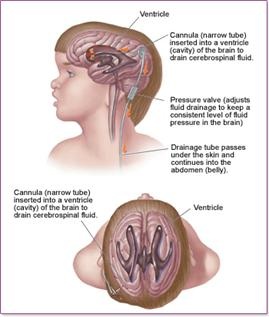
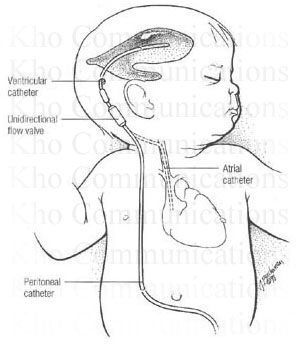
Hydrocephalus
Hydrocephalus is a disorder in which excess cerebrospinal fluid (CSF) accumulates within the cerebral ventricles and/or subarachnoid space. Essentially, there is an imbalance between the CSF outflow and inflow somewhere along the line or the body is not absorbing the CSF like it should. This can lead to a backup of CSF causing the ventricles to expand. Congenital Hydrocephalus is associated with an increased intracranial pressure (ICP) and usually present in the pediatric population. With Normal Pressure Hydrocephalus (NPH), there isn't an increase in ICP but rather there is an impairment in the CSF absorption. NPH is more commonly seen in the adult population. Congenital hydrocephalus has a prevalence of 0.8 per 1000 births. Hydrocephalus is believed to have both an absorption component and an obstructive component which cause the CSF flow issues.
|
Presentation:
In Normal Pressure Hydrocephalus, much of the presentation is similar. However, there are three cardinal signs:
|
Risk Factors:
Patients with congenital hydrocephalus have a strong association with Spina Bifida (~ 50%) Recommendation:
Refer out when an undiagnosed hydrocephalus is suspected. Remember: Normal pressure hydrocephalus does not have the same obvious presentation as congenital hydrocephalus. However, this form is more likely to occur in adults, especially following traumatic events to the head. |
|
Diagnosis:
Confirmed through imaging
|
Differential Diagnosis:
Congenital hydrocephalus should be examined for associated anatomical abnormalities:
Normal Pressure Hydrocephalus (NPH):
|
Shunt Dysfunction
Shunting is the main form of treatment with hydrocephalus, especially obstructive hydrocephalus. The shunt is placed to prevent accumulation of excess CSF in the brain and instead allows it to bypass the obstruction. The CSF can then flow back into the systemic system.
|
Diagnosis:
CT scans are not always reliable, especially with NPH. Instead, research suggests close monitoring of the signs and symptoms by the therapist as well as regular follow-up appointments with the PCP. |
Risk Factors:
40% of complications occur during the first year of the shunt surgery though shunt malfunctions can be a lifelong risk. |
|
Signs & Symptoms of Shunt Dysfunction:
|