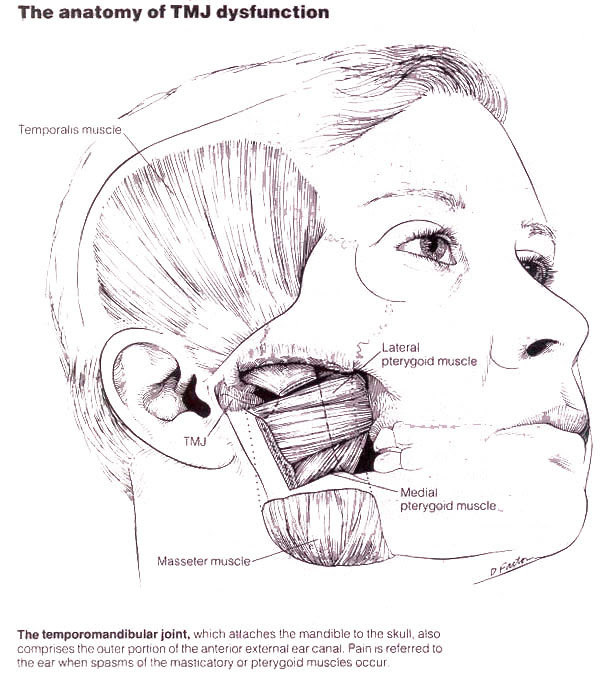
Temporomandibular Joint Dysfunction (TMD)
TMDs include musculoskeletal and neuromuscular conditions that involve the temporomandibular joints (TMJs), the masticatory muscles, and all associated tissues. Common painful TMDs are generated from myogenous and/or arthrogenous components. A painful TMD may occur in 10% of the population and other signs and symptoms of TMD (eg, clicking, limited range of motion, pain on function) have been reported in 46.1% of the United States population.6,7 Studies of non-patient populations have found that up to 75% of people studied have at least one sign of joint dysfunction and nearly one-third of the population has at least one TMD symptom.
Headaches and TMD are common and may therefore be reported as a single or as separate entities. The TMJ, masticatory muscles, and associated orofacial structures may act as triggering or perpetuating factors for primary headache. A primary headache disorder may similarly trigger or perpetuate pain in the masticatory muscles or TMJ. Ciancaglini and Radaelli3 reported that headache occurs significantly more frequently in patients with TMD symptoms (27.4% vs 15.2%). Individuals with myogenous TMDs are more likely than those with arthrogenous TMDs to have headache, and the prevalence of TMD in patients with migraine and tension-type headache is higher than in a nonheadache population.
The potential for headache secondary to TMDs is also is also seen. Jaw movement or pressure applied to the TMJ or surrounding musculature frequently exacerbates the secondary headache. The described pain typically manifests ipsilaterally when the TMJ is the pain generator, but may be bilateral with muscular involvement. Peripheral and central mechanisms are likely involved in myogenous TMDs. Painful TMDs may increase central sensitization, inducing, exacerbating, or contributing to the chronification of headache. Regardless of whether or not evidence of causation can be shown, ignoring TMDs as peripheral triggers of headache often results in a poor clinical outcome.
Headaches and TMD are common and may therefore be reported as a single or as separate entities. The TMJ, masticatory muscles, and associated orofacial structures may act as triggering or perpetuating factors for primary headache. A primary headache disorder may similarly trigger or perpetuate pain in the masticatory muscles or TMJ. Ciancaglini and Radaelli3 reported that headache occurs significantly more frequently in patients with TMD symptoms (27.4% vs 15.2%). Individuals with myogenous TMDs are more likely than those with arthrogenous TMDs to have headache, and the prevalence of TMD in patients with migraine and tension-type headache is higher than in a nonheadache population.
The potential for headache secondary to TMDs is also is also seen. Jaw movement or pressure applied to the TMJ or surrounding musculature frequently exacerbates the secondary headache. The described pain typically manifests ipsilaterally when the TMJ is the pain generator, but may be bilateral with muscular involvement. Peripheral and central mechanisms are likely involved in myogenous TMDs. Painful TMDs may increase central sensitization, inducing, exacerbating, or contributing to the chronification of headache. Regardless of whether or not evidence of causation can be shown, ignoring TMDs as peripheral triggers of headache often results in a poor clinical outcome.
|
Signs/Symptoms:
|
Causes:
|
|
Criteria for Diagnosis:
i. Any headache fulfilling criterion iii ii. Clinical and/or imaging evidence of a pathologic process affecting the TMJ, muscles of mastication, and/or associated structures iii. Evidence of causation shown by at least 2 of the following:
|
|
Physical Therapy Implications:
A physical therapist develops programs for patients that includes learning and practicing techniques for regaining normal jaw movement. The focus of physical therapy for TMD is to teach relaxation, stretching, and releasing tight muscles and scar tissue. Physical therapy techniques may include:
|
When to Refer:
|